A state law that hasn’t changed since 1975 caps compensation for families harmed by medical negligence. The limits apply to lost quality of life, even if a patient loses a leg, a child, or is disabled for life. Click on the picture of the map to find patients by the State Senate Districts they live in.
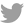
Shilpa Airy
San Francisco, CA
Assembly District 19, PatientsForFairness, Senate District 11
Assembly District 19, PatientsForFairness, Senate District 11
Shilpa Airy was an entrepreneur and research scientist who ran a successful biotech consulting business in San Francisco. She worked with many of the top researchers and physicians around the world. She was a leader in her field and devoted her career to developing medications to treat or cure diseases. She was especially proud of an FDA-approved drug she worked on to treat a rare genetic disease in children.
Shilpa befriended everyone. When she walked into a room, everyone knew who she was. She was a force of nature.
From a family of academics and scientists, Shilpa worked her way through college. After a brief stint in the corporate world, she decided she could help more people if she opened her own business. So, she moved to California and started her company.
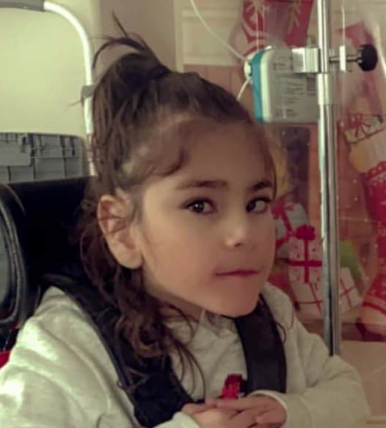
Her world came to a screeching halt in 2014 when Shilpa had routine gall bladder surgery. A week following the procedure she began having severe abdominal pain. Shilpa reported to the ER, where they ordered a CT scan, but a known allergy to the dye they used during the scan caused her to begin vomiting immediately afterwards. She was admitted to the hospital and scheduled for an exploratory endoscopy. At the start of the endoscopy, Shilpa’s airway was not protected and she breathed vomit into her lungs. She ended up in a coma with complete lung failure. She was on multiple forms of life support for nearly a month.
Although Shilpa showed all the signs, her providers failed to see that she had acquired an intestinal infection involving C-Difficile, likely acquired during her previous hospitalization. Had the infection been treated with antibiotics promptly, instead of attempting an endoscopy on a patient with active vomiting, she would not have suffered lung damage.
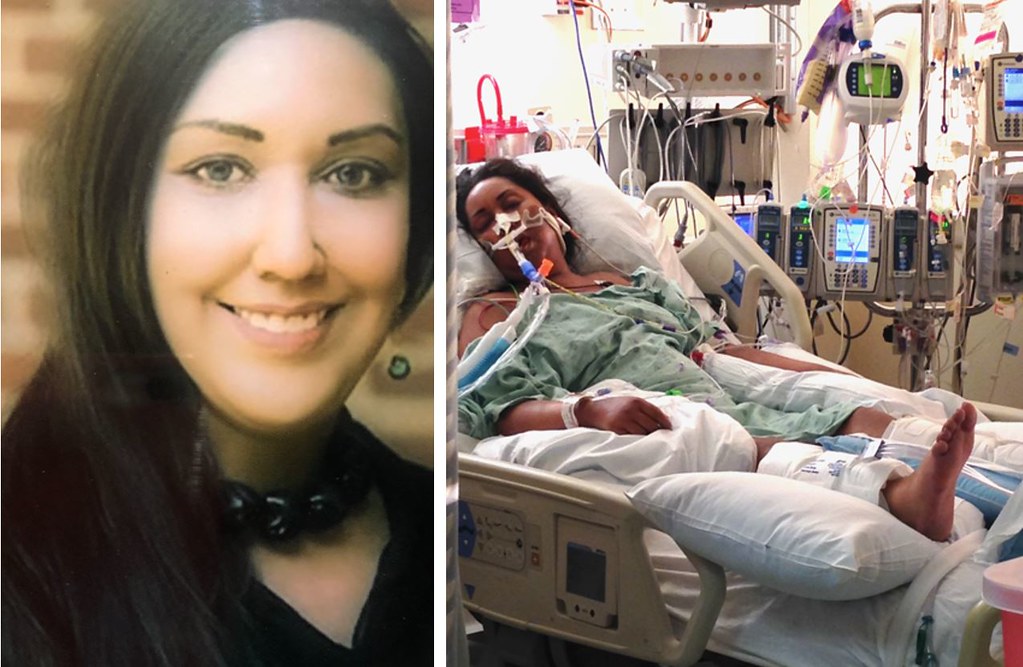
It was a miracle Shilpa survived but she was now home bound and reliant on her sister as a caregiver.
Her severely damaged lungs never recovered beyond 30%, and she was forced to use oxygen 24 hours a day. Over the next four years, her lung damage caused heart complications, but Shilpa’s repeated requests to see a specialist were also denied. Her condition declined to the point that she could no longer speak. During these four years, Shilpa was evaluated and monitored by lung transplant specialists but they chose not to list her until it was too late. Only two months before her death, she was diagnosed with severe high blood pressure in the lungs and end-stage heart failure, conditions that her team of five lung transplant specialists should have been able to catch months, if not years, earlier. The heart condition developed as a result of her lung damage. She was finally placed on the lung transplant list one month before she died. Shilpa didn’t just experience one medical mistake. She survived a series of mistakes but ultimately died from medical negligence at two different hospitals.
Shilpa worked with renowned doctors and devoted her career to finding cures for others. Yet, as hard as she tried, she was unable to survive medical negligence. She was a happy, positive woman, but her deteriorating condition broke her spirit.
Shilpa wanted the medical providers whose negligence destroyed her lungs and later her heart to acknowledge their errors and improve patient care. She filed a lawsuit while she was still alive. But a law passed by politicians in 1975 caps compensation in cases of medical negligence. Because of California’s outdated law, providers are not held accountable for preventable errors.
One of Shilpa’s medical providers settled her case while she was still alive, but she died before the full case was heard. Under the 1975 law, the value of a young person’s life was capped at $250,000 and has not been updated in the 45 years since it was enacted. The harsh reality is that Shilpa’s case was more valuable while she was still alive. Once she died, her family could not recover medical expenses or her extensive lost earnings, not even her funeral expenses.
To date, none of Shilpa’s medical providers at both hospitals have apologized for their negligence.
Like Shilpa, her family just wants accountability for her death. Because the law caps their recovery, they will not get it for any reimbursement of her medical expenses. Her family is left without an extraordinary sister and daughter, and the world is left without a researcher to develop a cure for disease.
In her lifetime, Shilpa fought for a cure for other Californians. “Shilpa would want accountability and justice for others,” said her sister Alka. This is what drives her sister and her family to support updating the 1975 limits on compensation for patients killed by medical negligence. “It is what Shilpa would have wanted.”
Californians will have the chance to vote on the Fairness for Injured Patients Act on the November 2022 ballot. The Fairness Act would update California’s medical malpractice damage cap for nearly 50 years of inflation, and allow judges and juries to decide fair compensation in cases involving catastrophic injury or death. Learn more about this campaign for patient safety.
Meet more patients
Screen Shot 2021-06-14 at 12.22.14 PM
Screen Shot 2021-06-11 at 5.16.55 PM
Screen Shot 2021-06-11 at 4.50.16 PM
Screen Shot 2022-04-06 at 12.58.49 PM
AnonymousR
Screen Shot 2021-06-11 at 2.04.15 PM
Screen Shot 2021-06-11 at 2.35.48 PM
Screen Shot 2021-06-14 at 3.01.10 PM
Paid for by Consumer Watchdog Campaign for the Fairness for Injured Patients Act
Committee Major Funding from:
Consumer Watchdog Campaign Nonprofit 501(c)(4)