A state law that hasn’t changed since 1975 caps compensation for families harmed by medical negligence. The limits apply to lost quality of life, even if a patient loses a leg, a child, or is disabled for life. Click on the picture of the map to find patients by the State Senate Districts they live in.
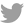
Don Stegman
Grover Beach, CA
Assembly District 35, PatientsForFairness, Senate District 17
Assembly District 35, PatientsForFairness, Senate District 17
After forty years of marriage, Don and Jill Stegman had it all—two beautiful children, a stable relationship, fulfilling careers. But a blood cancer led Don to a bone marrow transplant in 2007. Recovery over the next several years included frequent bouts of graft-versus-host disease, which was treated with a drug called prednisone.
Prednisone is a corticosteroid, a potent inflammation fighter for many types of illnesses and diseases from rheumatoid arthritis to glaucoma. In fact, over 55 million prescriptions a year are written for this drug. But while it is a life-saver for many, it comes at a terrible cost for those who must stay on high doses for prolonged periods of time. Long-term use can lead to heart disease, kidney disease, osteoporosis, diabetes, and psychiatric reactions. Don was prescribed high doses of prednisone on and off for several years following the bone marrow transplant for flareups of graft-versus-host disease.
Although Don’s doctors seemed to be on top of the physical problems Don experienced from prednisone, Jill was concerned about Don’s mental deterioration while he was on the drug. During this time Don became initially euphoric, then had insomnia, and finally “crashed and burned,” acting erratic and combative. Don had never been that way. Jill and Don always had a close relationship, hiking the hills around their home in Atascadero, biking the country roads, and walking on the beach in Morro Bay. Now Don seemed like a stranger who could barely tolerate Jill’s presence.

These symptoms usually subsided when Don was tapered to lower doses of prednisone, but in 2013 Don suffered a severe development of pneumonia and had to be treated with prednisone again. This time Don reacted with severe psychiatric symptoms. He became paranoid and particularly combative. He was told to leave a local pharmacy when he became frustrated with a prescription refill. He refused to eat Jill’s meals, saying her food “tasted funny” and that it contained ingredients he wasn’t supposed to be eating, even though his doctors hadn’t prescribed any food restrictions.
Jill knew that she had to get help for Don, and his doctors were her only hope since he refused to get help on his own. She was so concerned that she called his local oncologist’s office and reported that Don was “a danger to himself and others,” which is supposed to be a warning that requires immediate response, but Don’s oncologist never called Jill back. In fact, he never even mentioned Don’s mental health on the next visit.
Jill was in despair. From her research she read that psychiatric problems were common in people on corticosteroids like prednisone. Studies indicated that actual mood disorders could occur as well as depression. Jill read that patients on prednisone could become suicidal. Don’s doctors should have known this information since they commonly treated patients with high doses of prednisone. They had seen Don when he was acting aggressively. One had even commented that his behavior was “scary.”
The studies said that close monitoring of patients for psychiatric problems was crucial and that patients should be tapered from the drug if possible and be placed under psychiatric care if symptoms did not decrease. Specific drugs were recommended for treatment of psychiatric conditions that persisted during the tapering off period.
Jill called Don’s doctor and described Don’s mental instability and that he needed immediate intervention. By then Don had instigated a confrontation with a parking lot attendant at the hospital and his doctor had been informed about the incident. The doctor acknowledged that Don had a problem but refused to prescribe any drugs or call for a psychiatric evaluation, saying that “Don will be fine” once he was tapered off the prednisone, which would take months. The doctor had no other advice for Jill.
Over the next months Don did change. He became less angry and irrational, but he wasn’t normal. Jill noticed that Don didn’t get the same enjoyment out of his life. He became quiet and withdrawn. But Jill kept thinking he’d return to normal because Don’s doctor had assured her with the words, “If we just taper him off the prednisone, he’ll be fine.”
On a bright day in November, Don and Jill went for a stroll on their favorite beach with their little dog. Their son, John, was completing his law school studies and their daughter, Anna, was home from college. Don stared out at the wind surfers performing their acrobatic maneuvers in the waves. He’d been an avid surfer himself until recently when various medications had affected his balance. Don looked at Jill solemnly and admitted that he was very depressed. He agreed to get help.

Jill stuck by Don over the weekend until the next business day, when doctors’ offices were open. She called Don’s doctors first but received no help. Don’s primary care physician told her the doctor didn’t see patients for depression and suggested calling psychiatrists’ offices, but none of them took Medicare. The local oncologist’s receptionist told her that the doctor didn’t see patients for depression. Jill felt an overwhelming sense of dread, realizing that she was on her own in finding mental health assistance.
After two hours of calling, Jill wasn’t able to locate a psychiatrist for Don. They either weren’t taking new patients or they didn’t take Medicare. Suddenly Don rose from the kitchen table and ran out the door to the garage. Jill heard the truck pull away.
Jill continued calling, hoping that Don would soon return. He had disappeared before during the last few months. She finally stopped calling at noon, when most doctor’s offices were closed for lunch. Don had now been gone for several hours.
Sensing impending doom, Jill waited through the afternoon. She finally called the police to report that her depressed husband had been missing all day. Late that night two sheriffs knocked on her door. They reported that Don’s body had been found. He’d shot himself in the head with his grandfather’s old shotgun.
Jill began contacting medical malpractice attorneys, not as a way to seek vengeance against a medical establishment whose dismissal of Don’s symptoms led to his death, but rather to hold these medical professionals accountable and prevent this kind of neglegience from happening to others. Many attorneys listened to Jill and agreed that she had legitimate cause for a medical malpractice lawsuit. However, none would take her on because of the 1975 California law that limits the wrongful death component of medical malpractice lawsuits to only $250,000 — so low that it would have cost as much to take Don’s case to trial as any potential recovery.
Californians will have the chance to vote on the Fairness for Injured Patients Act on the November 2022 ballot. The Fairness Act would update California’s medical malpractice damage cap for nearly 50 years of inflation, and allow judges and juries to decide fair compensation in cases involving catastrophic injury or death. Learn more about this campaign for patient safety.
Meet more patients
Screen Shot 2021-06-11 at 4.50.16 PM
Screen Shot 2021-06-14 at 4.24.22 PM
Screen Shot 2021-06-14 at 2.21.06 PM
Screen Shot 2021-06-14 at 3.10.10 PM
Screen Shot 2021-06-14 at 3.03.24 PM
Screen Shot 2021-06-14 at 3.23.58 PM
Screen Shot 2021-06-14 at 12.22.14 PM
Screen Shot 2021-06-11 at 2.04.15 PM
Paid for by Consumer Watchdog Campaign for the Fairness for Injured Patients Act
Committee Major Funding from:
Consumer Watchdog Campaign Nonprofit 501(c)(4)